D Symptoms Secondary To Bile Duct Obstruction
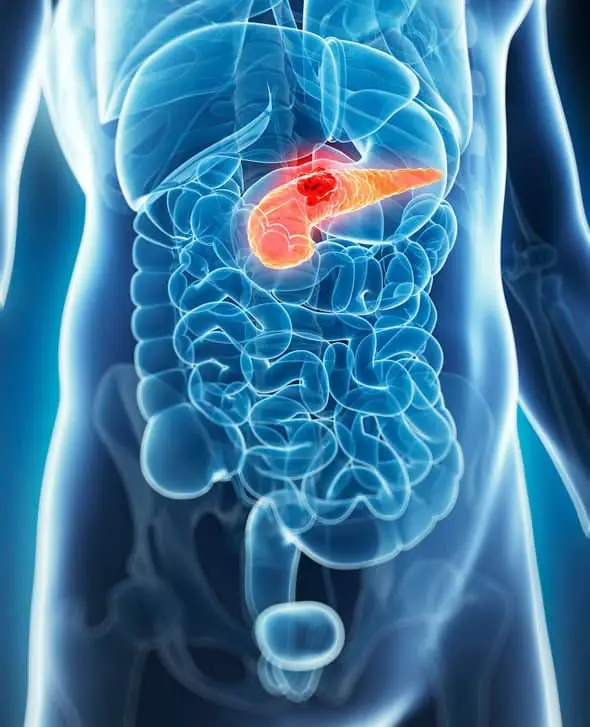
Because the pancreatic tumor mass of ductal adenocarcinoma most commonly arises from the head of the pancreas which are the sections where the bile duct joins with the pancreatic duct, the normal flow of the bile duct is often obstructed, thus disrupting the natural deposition of the bile fluid into the small bowel. This bile duct obstruction causes a back-up of the bile pigment into areas where it shouldnt normally go creating the clinical symptoms of jaundice with its attendant yellowish skin coloration and other associated changes, and which is often accompanied by a loss of appetite and by the symptom of unrelenting and often debilitating pruritis of the skin.
Additionally, the lack of bile salts which are now unavailable for normal digestive and other bowel processes, can result in complex physiological interactions leading to liver and immune dysfunction. This interruption of normal bile deposition may also disrupt the absorption of fat-soluble vitamins and the conjugation of endotoxins, thus leading to possible blood coagulation difficulties, malabsorption syndromes and even kidney failure. Also, up to ten percent of affected patients may develop cholangitis .
What Are The Other Signs And Symptoms Of Pancreatic Cancer
The signs and symptoms of pancreatic cancer may also be found in other conditions of the digestive system. These include
- Yellowish discoloration of the skin and eyes
Unusual signs include
- Fatigue: fatigue is a common symptom found in other types of cancer as well.
- The new and unusual onset of diabetes: Pancreatic cancers may destroy the insulin-producing cells. This can increase your blood sugar levels and lead to newly diagnosed diabetes. If you already suffer from diabetes which is under control, you may suddenly develop an uncontrolled form of diabetes.
What Can I Do
- Tell your doctor or nurse as much as you can about your pain. This will help them give you the right treatment.
- It can help to keep a diary of your pain to share with your doctor or nurse.
- Take your pain relief as advised by your doctor. This will help to make sure it works as well as possible.
- Speak to our specialist nurses on our free Support Line with any worries.
Also Check: What Causes Severe Pain In Lower Right Side Of Back
Pain Management For Pancreatic Cancer Patients
One of the earliest and most common side effects of pancreatic cancer is pain. The pancreas sits below your sternum in your mid-abdomen and is surrounded by several other organs and nerves. As tumors on the pancreas grow, they often push against these other body parts, which can be very painful, says pancreatic cancer researcher Shubham Pant, M.D.
Pain can be isolated to the abdomen, or travel to your lower back, and can be quite uncomfortable. It can also impact a patients quality of life and lead to challenges during cancer treatment.
When youre in pain, you dont sleep well. You may not eat well, and you can become depressed, says cancer pain specialist Shalini Dalal, M.D. Here, Dalal and Pant share insights on pancreatic cancer pain.
Bloating and back pain are common pancreatic cancer pain symptoms
As a pancreatic tumor grows, patients may feel bloated. Patients may also experience nerve pain in their back as the tumor presses against a bundle of nerves in the upper abdomen known as the celiac plexus.
However, pancreatic cancer-related pain is often mistaken for other conditions like acid reflux or indigestion, which can delay diagnosis. When patients receive a pancreatic cancer diagnosis, theyve often been in pain for some time, Pant says.
Pain management can influence treatment success
Managing pain effectively can lead to weight gain, relieve constipation and help you get the rest you need during cancer treatment.
Advice for patients with pancreatic cancer
Whats The Outlook For People With Back Pain And Cancer
Less than 10 percent of spinal tumors actually start in the spine, according to the Memorial-Sloan Kettering Cancer Center. Even if a spinal tumor is present and causing lower back pain, the tumor isnt always cancerous.
If the lower back pain is related to metastatic cancer, its important to talk to your doctor about your treatment outlook. When cancers start to spread, this may indicate a poorer prognosis.
Also Check: What Do Chiropractors Do For Lower Back Pain
Moderate To Severe Pain
The most common medications used for advanced pancreatic cancer pain are stronger opioids. These include, among others, morphine, hydromorphone, fentanyl, and methadone.
Like other categories of pain treatment and dosing, finding the right combination involves trial and error. Your doctor may start you at a lower dose and then increase the dose until your pain is controlled. Additionally, other drugs or therapies may be added to help control pain and reduce the amount of strong opioid needed for pain control.
As with all treatments, be sure to tell your doctor if your pain is not being controlled, even with stronger medications. Theyll likely change the dose, or the treatment, so you are more comfortable.
One thing to watch for is called breakthrough pain. As the name implies, this situation occurs when your pain is controlled most of the time but you experience periods of pain before your next scheduled dose of pain medication. In some cases, this means a higher overall dose is needed. There may also be other ways to help manage breakthrough pain.
Side effects that may occur with stronger opioids include:
In general, people taking opioids should avoid alcohol as it can add to the feeling of drowsiness. You should also avoid driving a car or performing other activities that require alertness until you know how you respond to these medications.
What Is Pancreatic Cancer
The word cancer means an uncontrolled and unregulated growth of cells. When cancer starts in the pancreas, it is called pancreatic cancer. The pancreas is an organ located in the upper left abdomen, behind the stomach. This organ serves several important functions, particularly regulating digestion and blood sugar levels. The pancreas has four main parts: head, neck, body and tail. Almost 75 percent of all pancreatic cancers occur within the head or neck of the pancreas, 15 to 20 percent occur in the body of the pancreas and 5 to 10 percent occur in the tail. When cancer develops in the pancreas, the rapidly-dividing cancer cells form a mass or tumor that can spread to other sites in the body. The cancerous mass deprives the normal cells of nutrition and space, causing a disturbance in the functioning of the pancreas.
According to the American Cancer Society, about 60,430 people in the US will be diagnosed with pancreatic cancer in 2021. Also, pancreatic cancer will cause about 48,220 deaths in the US in 2021.
Read Also: What Can You Do To Help Lower Back Pain
Symptoms Of Endocrine Pancreatic Tumours
Endocrine pancreatic tumours are uncommon. They are also called neuroendocrine tumours. Most pancreatic neuroendocrine tumours don’t produce hormones so don’t cause specific symptoms.
Pancreatic neuroendocrine tumours that produce hormones are called functional tumours. The symptoms are different for each type, depending on the hormone the tumour produces.
What Are The Symptoms That Affect The Digestive System
Pancreatic cancer comes with some sneaky symptoms that can affect your digestive system. Since some of these symptoms are common, it can be hard to recognize that they could be caused by pancreatic cancer. Of course, just because you have one or more of these symptoms doesnt mean you should make assumptions about having cancer. Keep an eye on them and if any of these symptoms persists, fill in your doctor.
- loss of appetite
Also Check: Do Corsets Help Back Pain
What Back Pain Treatment Options Are Available To Me What Type Of Back Pain Is Associated With Pancreatic Cancer
There are many methods for treating back pain at home, but only a few of these have been proven to be effective. The most common treatment is rest and applying ice to the painful area. This treatment is very relaxing and should be used for only 10-20 minutes. It should never be applied while you sleep. Also, exercise and stretching exercises are essential for keeping muscles and supporting tissues flexible. While some of these methods may not seem like they are effective for you, they can help you overcome your back pain.
Physical therapy is a good option for treating back pain. It will help you improve your posture and strengthen your core muscles. Massage therapy and acupuncture are other options for relieving tension and reducing joint pain. Some people also find that water therapy improves flexibility and balance, while yoga helps them heal faster from injuries. Proper nutrition and lifestyle changes are also important for treating back pain. It is very important to consult a physician if you are experiencing back pain because it will help you avoid more serious conditions later on.
Triggers To Seek Help For Intermittent Symptoms
Although Marcus recognised that his indigestion with fever recurred several times in similar circumstances, this alone was not enough to make him seek medical help. However, others did. Drawing on social science theories of consultation behaviour we have identified specific triggers to seeking help when symptoms have been intermittent. Such symptoms were rarely acted on until a pattern became apparent, the frequency of symptom episodes increased, there was a change in the nature of the intermittent symptoms or additional symptom appeared. We illustrate these triggers below.
A pattern became apparent
Paddy also recognised that his repeated bouts of severe abdominal pain followed a pattern, but because they always occurred at night he did not see a doctor until the pain had disappeared.And part of the early days that I remember was the sort of oddity of having these pains which they, if they started at say 7 o’clock in the evening, they followed a particular course till about sort of 2 or 3 o’clock that morning. They were absolutely the same each time. But they never seemed to happen when I could quickly get to a doctor. And one of the early sort of irritations I remember of this problem was that I never seemed to be able to get to a doctor when I was actually in the pain. So by the time I actually saw a doctor, perhaps the next morning if I was lucky, or a few days later, the pain had gone.
Increased frequency of symptoms
Change in the nature of the intermittent symptom
You May Like: How To Ease Lower Back Pain Fast
What Are The Risk Factors For Pancreatic Cancer
Pancreatic cancer can affect anyone. The presence of certain risk factors, however, makes someone more vulnerable to get the disease. Nonetheless, the presence of risk factors does not mean that the person will surely get the disease. Likewise, the absence of risk factors does not make one immune from getting pancreatic cancer.
Some of the major risk factors for pancreatic cancer include
- Non-modifiable risk factors: These include the risk factors that are not in ones control and they cannot be changed. They include
- Age: Pancreatic cancer risk increases as a person grows older. Most people affected by this cancer are older than 45 years of age with almost 75 percent of patients being at least 65 years old.
- Gender: The number of pancreatic cancer cases is higher in males than in females.
- Race: African-Americans seem to be at a higher risk than Caucasians.
- Genetic syndromes: Certain inherited conditions, such as hereditary breast and ovarian cancer, may increase the risk.
- Family history: A history of pancreatic cancer in a parent, child or sibling may increase the risk of the disease although most patients diagnosed with the condition do not have a positive family history.
Pancreatic Cancer Pain Management
Comprehensive Pain Assessment
Your physician will conduct a comprehensive pain assessment to determine:
- When the pain started
- Where the pain is located
- How intense the pain is
- How various cancer treatments have impacted your pain level
Following the assessment, your doctor will help devise a treatment plan designed to maximize your comfort.
You May Like: How To Treat A Torn Disc In Lower Back
Stomach And Back Pain
A common symptom of pancreatic cancer is a dull pain in the upper abdomen and/or middle or upper back that comes and goes. This is probably caused by a tumor that has formed in the body or tail of the pancreas because it can press on the spine.
Some patients describe pain starting in the middle abdomen and radiating into the back. Pain can be worse when lying down and can often be relieved by leaning forward. Pancreatic cancer pain can differ from person to person, so be sure to discuss any new pain-related symptoms with your doctor.
Back Pain Can Signify Serious Health Issues
In some cases, however, back pain could also mean a serious health issue such as pancreatic cancer. Pancreatic cancer develops in the tissues of the pancreas – an organ in the abdomen that lies behind the lower part of your stomach.
According to a report by the All India Institute of Medical Sciences , the cases of pancreatic cancer in India is on the rise. The incidence of pancreatic cancer in India is 0.5-2.4 per 100,000 men and 0.2-1.8 per 100,000 women. It is the 11th most widely prevalent cancer in the country and has an extremely low survival rate if undetected and un-operated at the initial stage, says the doctor.
Read Also: Should I See A Chiropractor For Back Pain
What Are The Symptoms Of Pancreatic Cancer
Pancreatic cancer often doesnt cause symptoms in the early stages. As the cancer grows, it may start to cause symptoms. The symptoms may not be specific to pancreatic cancer, and they may come and go to begin with. This can make pancreatic cancer hard to diagnose.
These symptoms can be caused by lots of things, and are unlikely to be pancreatic cancer. If you are not feeling well and you have any of the symptoms on this page, speak to your GP to check if there is anything wrong.
Common symptoms include:
Pancreatic Cancer Pain: Impact And Management Challenges
Accepted for publication 2 March 2017
24 May 2017Volume 2017:7Pages 1317
Wesley B Jones,1 Allyson L Hale2 1University of South Carolina School of Medicine Greenville, Greenville, SC, USA 2Department of Surgery, Greenville Health System, Greenville, SC, USA Abstract: The majority of patients with pancreatic cancer experience a pain that will significantly alter their quality of life. Based on the low survival rates associated with pancreatic cancer, management of pain is an important component of palliation. Current management options include medication and intervention, specifically celiac plexus neurolysis and bilateral thoracoscopic splanchnicectomy . The purpose of this paper is to outline the current state of interventional palliation of pain associated with malignant neural involvement in patients with pancreatic cancer. At present, CPN and BTS are not typically used until after failure of narcotic medications, even though narcotics have numerous side effects. Multiple studies have evaluated CPN or BTS and shown excellent outcomes for pain control, with 60%90% successful palliation. Moreover, few complications have been reported in the literature. Because of the side effects commonly experienced with narcotics, as well as the high success and low complication rates of intervention, most authors recommend early intervention by way of BTS or CPN for patients with pancreatic cancer in significant pain. Keywords: splanchnicectomy, celiac neurolysis, pancreatic cancer
Recommended Reading: How To Relieve Lower Back Inflammation
The Course Of A Cancerous Spinal Tumor
Cancer is more likely to occur with age.3 People who are older than age 50 or previously had cancer are at an increased risk of developing a cancerous spinal tumor.1
A cancerous spinal tumors rate of growth can vary depending on the type. A tumor may be relatively small and contained within the spine, or it could have already spread through blood or lymph from another area of the body. An untreated cancerous spinal tumor is likely to keep growing and may become life-threatening.
Treatment options for spinal cancer may include radiation therapy, chemotherapy, immunotherapy, and/or surgical removal of the tumor. In cases when the patient is unlikely to tolerate surgery well or has advanced cancer, palliative care may be offered to reduce pain and stay as comfortable as possible, rather than removing the tumor.
Strengths And Limitations Of This Study
-
As is appropriate for this qualitative approach, we aimed for maximum variation and not numerical representation we included people with a wide range of backgrounds and experiences, not just those who had particular concerns about their prediagnostic symptom experiences or diagnostic delay.
-
The finding on intermittent symptoms emerged during analysiswe did not ask specifically whether symptoms occurred intermittently.
-
Our study is based on people’s recall of events, which is considered a bias in some research traditions, yet these accounts also emanate from those who, having been diagnosed with a life-threatening illness, are likely to have thought long and hard about how and when their cancer started. Using qualitative, interpretive methods allows us to analyse and learn from these recollections.
Don’t Miss: What Type Of Doctor Treats Back And Neck Pain
Elaine Did Not Have Jaundice But She Noticed That She Had Putty
I noticed something odd happening about five months before I actually went to the GP. And it happened about three times that I had, I was getting an increasing amount of sort of wind almost and burping a lot. That was the other thing that was very odd. And my husband said, Thats very odd. And then Id notice a few days later, sometimes I, each, each time I felt a little bit nauseous for a couple of days and then Id pass a very abnormal coloured stool, as if Id got a gallstone or something, if anybody else recognises those symptoms. I wasnt jaundiced, but I just had this very funny stool, which was almost putty coloured. And I thought, Well, that is very odd. Then months, and I hadnt noticed at that time that actually I had been feeling a little bit nauseous before. But the next time it happened when I was a bit nauseous and I think, Well, I wonder if the same thing will happen again? And it did. But that was very near Christmas and I thought, Well, in my experience I know its no good going to ones GP round about Christmas. Ill go straight after Christmas and then things will be looked into properly.