How Do You Know If Pelvic Pain Is Serious
While not all pelvic pain is serious, seeking medical care when symptoms are severe is important. You should head to the nearest emergency room if:
- Pelvic pain is sharp, severe or sudden.
- Youâre unable to stand up straight.
- There is blood in your pee or poop.
- Youâre running a fever.
- Youâre pregnant or have been pregnant in the last six months.
Possible Causes Of Sij Dysfunction
This may be a sudden force or trauma or overuse with repetitive movements or positions.
- Collison when driving with the foot on the pedal
- Twisting and lifting
- Excessive stress post pregnancy
- Long term issues in knees, hips or ankle. (Producing one sided weakness0
- Landing heavily on one leg.
- Prolonged sitting-especially with twisting
Injury And Stress Fractures
Athletic individuals are prone to injuries and trauma. Repetitive mechanical movements, such as exercise or sports, can induce stress fractures in the lumbar and sacral bones. These fractures can cause severe low back pain.
Multiple lumbar stress fractures were the cause of chronic low back pain in a young cricketer. Pelvic pain arising from pelvic stress fractures is not unusual in enthusiastic female athletes. Such fractures usually go undiagnosed.
Thus, if you indulge in sports activities and suffer pelvic aches, you might consider an underlying stress fracture.
Recommended Reading: Can Colon Cancer Cause Lower Back Pain
Pelvic Pain: Symptoms Causes And Treatments
Brandi Jones MSN-Ed, RN-BC is a board-certified registered nurse who owns Brandi Jones LLC, where she writes health and wellness blogs, articles, and education. She lives with her husband and springer spaniel and enjoys camping and tapping into her creativity in her downtime.
Jason DelCollo, DO, board-certified in family medicine. He is associate faculty at Philadelphia College of Osteopathic Medicine as well as adjunct faculty with the Crozer Family Medicine Residency Program, and is an attending physician at Glen Mills Family Medicine in Glen Mills, Pennsylvania.
The pelvis is located in the abdominal area, below your belly button and between your hips. Pelvic pain can occur in women and men, and it can originate in the urinary, reproductive, gastrointestinal, and musculoskeletal systems.
Pelvic pain intensity varies based on the cause and can be sudden, constant, or come and go.
This article discusses pelvic pain, causes, tests, treatment, and when to see your healthcare provider.
FatCamera / Getty Images
Common Causes Of Lower Back Pain That Radiates To The Front Pelvic Area
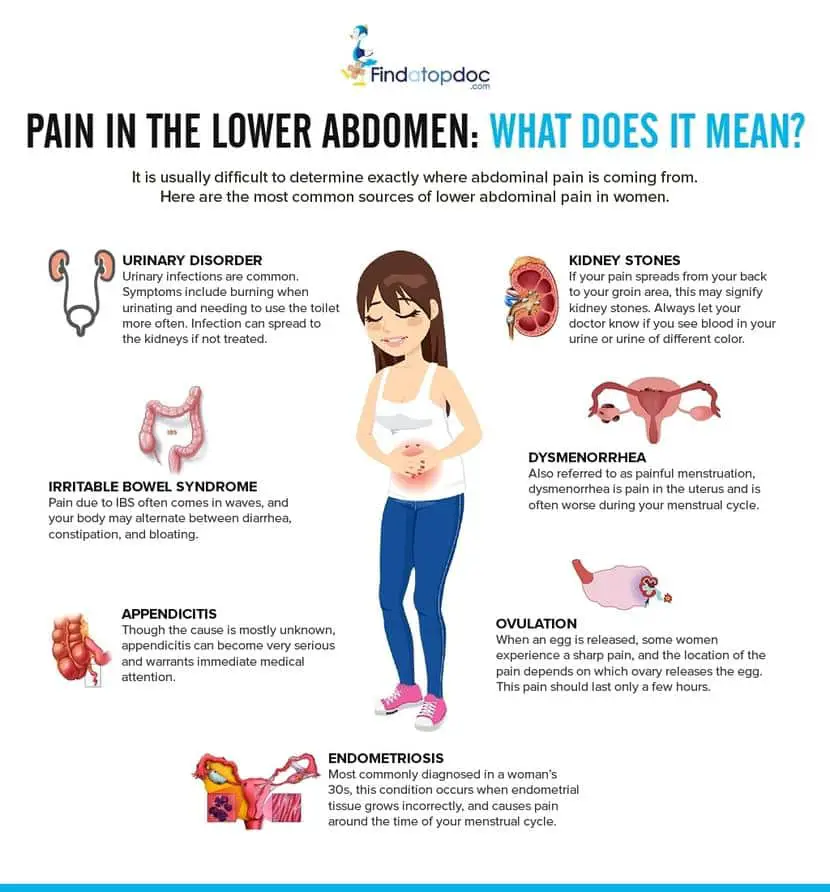
As lower back pain may cause referred pain in other parts of the body, including the front of the pelvis, its common to be misdiagnosedespecially if youre not seen by health care professionals who specialize in spinal-related issues.
Low back and front pelvic pain can come from many sources including:
- Bulging discs and nerve root irritation
- Sacroiliac joint injuries and pelvic dysfunction
- Physiological changes during pregnancy
- Generalized low back pain and facet joint injuries
A thorough examination can be used to figure out whether an individual’s pain is due to a problem with the spine, nerves, muscles, or sacroiliac joint. Physical therapists are well-versed in anatomy, biology, physiology, and kinesiology . This allows them to pinpoint areas of concern when symptoms are reported, such as lower back pain that radiates into the pelvis.
Don’t Miss: Why Is My Back In Pain When I Lay Down
Disc Injuries And Nerve Root Irritation
Treatment needs to be specific depending on your symptoms. Disc injuries with or without nerve root irritation can occur at any level in the spine. In its mildest form, a small broad based disc bulge is a normal part of aging and many of us will have this degenerative change without it causing pain. However, an acute focal disc bulge may cause inflammation that puts pressure onto the nerve root and this is often associated with referred pain, altered sensation, and difficulty weight bearing
Acute phase: Initially it is important to try to ease inflammation and pain, and to fully assess how the nerve is being affected.
Ongoing back or leg pain related to an old disc injury: There can be many reasons for ongoing symptoms that may linger long after the disc has healed or micro-discectomy surgery has repaired the protruded disc material. At this stage physiotherapy treatment should combine manual therapy to release over active muscles and improve nerve mobility, core and lumbo-pelvic muscle retraining to restore strength and endurance, and posture retraining to decrease any ongoing irritation of the nerve tissue and minimize the chance of re-injury
Physiotherapy post Lumbar micro-diecectomy +/- Lmainectomy
2. Pelvic dysfunction and Sacroiliac joint injuries
The Most Common Causes Of Lower Back Pain Are A Strain Or Sprain
Whether you notice it or not, your lumbar spine gets put to work throughout the entire day.
Amid all of this work and motion, a lower back sprain or strain can result from an acute injury, such as one experienced while falling, lifting something too heavy or playing sports. A sprain or strain can also develop over time due to repetitive movements or poor posture.
“Straining a muscle or spraining a ligament are the most common causes of lower back pain,” says Dr. Palmer. “While they can be serious, these common causes of lower back pain aren’t long-lasting taking anywhere from a few days to heal or, at most, a few months.”
Your doctor can help you determine the particular course of self-care that can help heal your lower back pain.
“The treatment for a pulled back muscle or strained back ligament is fairly simple and can include pain and anti-inflammatory medications, muscle relaxers, ice to help reduce inflammation, heat to promote healing, and avoiding strenuous activity until the pain recedes,” explains Dr. Palmer. “The best course of care will depend on the severity of your injury as well as your overall core and lower body strength.”
If your lower back pain persists despite treatment, it may be time to consider other causes of lower back pain.
Recommended Reading: What Kind Of Dr For Back Pain
Screening For Colorectal Cancer
A colonoscopy is a common screening test for colorectal cancer. While youâre mildly sedated, a doctor inserts a small flexible tube equipped with a camera into your colon. If they find a polyp, they can often remove it right then. Another type of test is a flexible sigmoidoscopy, which looks into the lower part of the colon. If youâre at average risk, screening usually starts at age 45. Your doctor may also screen you with different kinds of take home stool cards.
How Is Pelvic Pain Diagnosed
Tests will be done to determine the cause of the pelvic pain. In addition, your healthcare provider may ask you questions regarding the pain such as:
-
When and where does the pain happen?
-
How long does the pain last?
-
Is the pain related to your menstrual cycle, urination, and/or sexual activity?
-
What does the pain feel like ?
-
Under what circumstances did the pain begin?
-
How suddenly did the pain begin?
Additional information about the timing of the pain and the presence of other symptoms related to activities such as eating, sleeping, sexual activity, and movement can also help your healthcare provider in determining a diagnosis.
In addition to a complete medical history and physical and pelvic exam, you may have other tests including:
Also Check: How To Cure Upper Back Pain Fast At Home
Low Back Pelvic & Sacroiliac Joint
Luckily, the majority of people will get better quickly with the right treatment and muscle retraining. It is therefore important to find practitioners who have a depth of knowledge in assessing the lumbar spine and pelvis as well as surrounding muscles and nerves, and who know how to treat the many different types of back pain. A thorough initial examination allows us to determine what the main sources of your pain and disability are, and this allows us to direct treatment appropriately. 85% of people will suffer low back pain at some stage in their lives.
Overuse Injuries And Trauma
Frequent use and repetitive movement patterns can lead to overuse injuries to muscles, ligaments, and joints. They could include:
- Exercises and physical activities, like tennis or golf, that require repetitive twisting and bending in the same direction.
- Frequently lifting of heavy objects or any movements that are repeated regularly.
Trauma can also lead to lower back and groin pain. Trauma could result from car accidents, falls, or sports accidents. Such trauma can inflict both acute and chronic injuries to the body, like strained muscles or broken bones. Depending on the type of trauma, the healing time and treatment needed can vary.
Both overuse and trauma injuries to the lower back or groin area can lead to weakness in the legs, tingling, numbness, pain, stiffness, or popping sensations.
You May Like: What Causes Bad Lower Back Pain
What Causes Fibroid Flare Ups
Fibroid pain may be mild or extreme, constant or just occasional. It can flare up during sexual intercourse, bowel movements, exercise, or your period. Pain often radiates down the leg. Discomfort may also result when an enlarged uterus puts pressure on adjacent organs, such as the bladder or bowel.
How Do I Get A Pelvic Pain Diagnosis
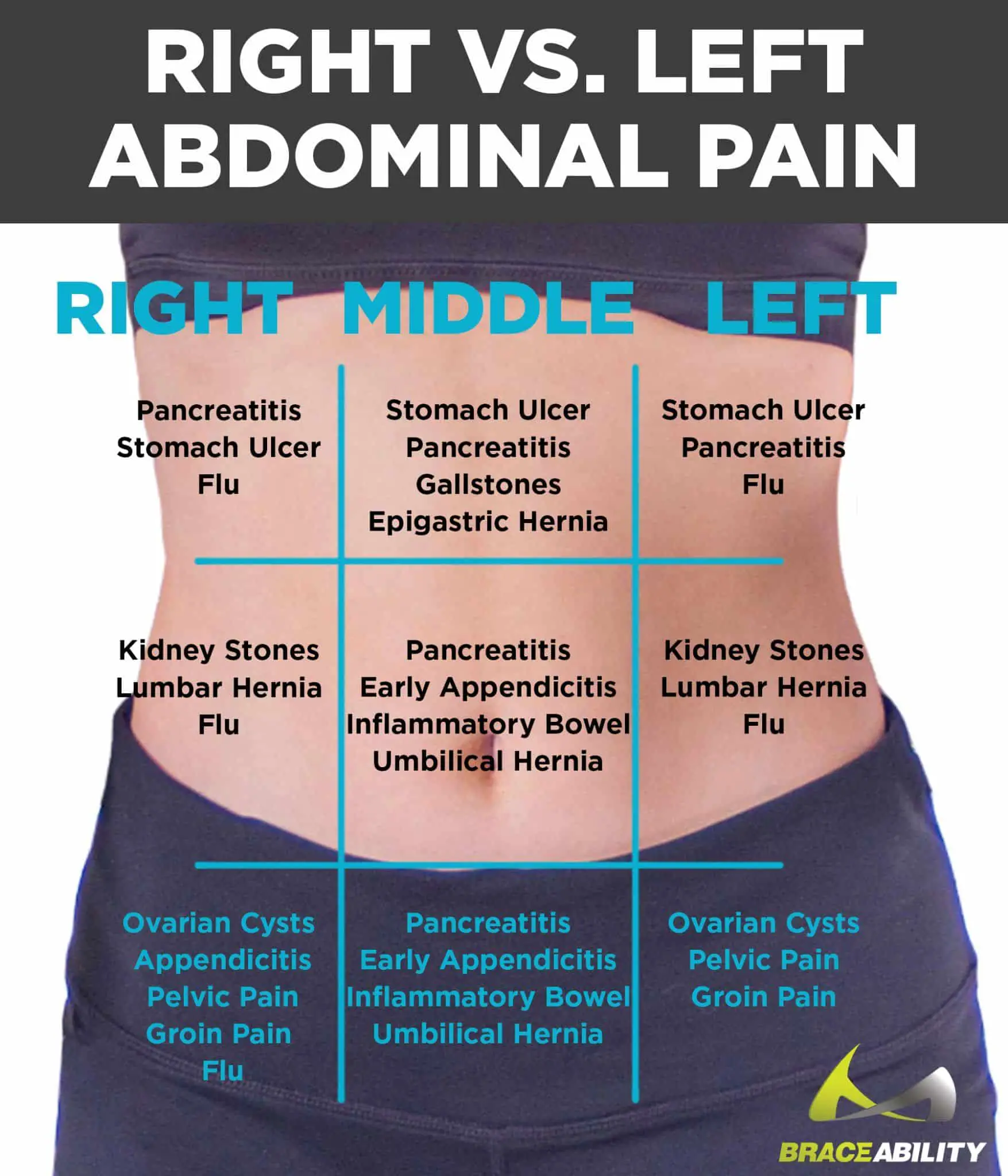
Pelvic pain is usually mild and settles by itself, but in some circumstances the pain can be complex and should be assessed by a medical professional or pain specialist, who will take the time to understand the pain story and perform a physical examination before setting forward a diagnosis and treatment plan.
In some circumstances imaging tests may be required. Types of imaging tests might be X-rays, CT scan, MRI scan, bone scan or ultrasound.
Once a pelvic pain diagnosis is made, the medical professional or pain specialist will determine the best treatment options.
Book an appointment to have a Pain Specialist make a pelvic pain diagnosis.
Read Also: How To Relieve Lower Back And Buttock Pain
How Is Pelvic Pain Treated
The treatment of pelvic pain depends on several factors, including cause, the intensity of pain and frequency of pain. Common pelvic pain treatments include:
- Medicine. Sometimes pelvic pain is treated with drugs, including antibiotics, if necessary.
- Surgery. If the pain results from a problem with one of the pelvic organs, the treatment might involve surgery or other procedures.
- Physical therapy. Your healthcare provider may recommend physical therapy to ease pelvic pain in some cases.
Living with chronic pelvic pain can be stressful and upsetting. Studies have shown that working with a trained counselor, psychologist or psychiatrist can be beneficial in many cases. Your healthcare provider can offer more information about various treatments for pelvic pain.
Treatment Of Pelvic Congestion Syndrome
Conservative management includes the use of compression devices such as medical-grade compression pantyhose or compression shorts
With the advent of advanced technology, patients can be treated using a minimally invasive procedure. The benefits of these procedures are:
- No hospital stays and usually can go home the same day.
- Small incisions and less blood loss.
- Less pain and no open surgeries.
- Minimal scarring and lower rates of complication.
- Treatment options may also include embolization of the ovarian vein and peri uterine veins. Risks during these procedures are minimal with a high success rate.
Outcomes of treatment allow patients to regain quality of life and may prevent the need for more invasive surgical treatment such as hysterectomy.
Also Check: What To Do For Neck And Back Pain
Causes Of Pelvic Pain And How To Relieve It
The pelvis is the area of the body below the abdomen. With many different organs and structures, such as blood vessels, nerves, the bladder, reproductive system and the bowel, there are many different causes of pain in the pelvis. And treatment will depend on the cause. Affecting both men and women, it might stem from infections, abnormalities in internal organs, or pain from the pelvic bones. In women, pelvic pain is often related to the reproductive system.
In this gallery, let’s discover possible causes of pelvic pain and how to relieve it. Click on for more.
How Can I Treat Pelvic Pain At Home
If you suffer from chronic pelvic pain, there are a few things you can do to ease symptoms at home. For example:
- Take over-the-counter pain relievers. Nonsteroidal anti-inflammatory drugs like ibuprofen or naproxen sodium can help reduce swelling that leads to pelvic pain. Acetaminophen can also ease painful symptoms.
- Make time for exercise. Even though you may not feel like moving, exercise helps increase blood flow and may help reduce your discomfort.
- Apply heat. Place a heating pad or warm compress over the area, or take a long soak in a hot bath.
- Stop smoking. Tobacco products can inflame nerves and cause pain. Avoiding these habits can help relieve pain.
- Take supplements. If your pelvic pain symptoms are due to vitamin or mineral deficiency, supplements could help soothe your discomfort. Talk to your healthcare provider before incorporating supplements into your daily routine.
- Practice relaxation exercises. Yoga, mindfulness or meditation can help reduce stress and tension. As a result, chronic pain may be eased.
You May Like: How To Treat Sciatica Lower Back Pain
Can Pelvic Pain Be Prevented
Pelvic pain canât always be prevented. However, incorporating these recommendations into your daily life can help reduce your risk:
- Donât overuse. Limit activities that require you to stand or walk for long periods of time.
- Eat more fiber. This is particularly helpful if your pelvic pain is due to diverticulitis.
- Exercise regularly. Staying physically active helps keep your joints and muscles in good condition.
- Stretch your muscles. Warm up before exercising to help reduce the risk of pelvic pain.
- Visit your healthcare provider regularly. Routine examinations can help your medical team detect issues early on before they worsen.
What Sets Us Apart
What sets our back pain treatments apart from so many others is the incorporation of our deep understanding of the nervosu system and how that translates into healing- it’s not just about changing the structure but also changing the pathways that connect the strcuture to the brain. And it’s this reconnection and reintegration that serve as the backbone of what we do. We are New England’s premier center for chiropractic neurology.
We understand that everything in the body is conected. From the spine to the brain, the nervous system is the engine of feeling. And when a connection is broken, you feel it. The connection and reintegration is the inspiration behind our care, demonstrating the core of who we are: restoring connections in our patients.
A person’s pain is a result of a combination of factors involving muscle, joint, nerve and brain. Thereby, a diagnostic and treatment approach that involves all of those structures will create the best possible, long-term outcome. That’s what the Portland Chiropractic Neurology model incorporates, reconnecting all of these structures through a multi-modal appraoch that combines chiropractic, physical therapy, occupational therapy, neurology and hyperbaric oxygen therapy. Our analysis allows us to determine which therapies are right for you and then applied over a certain treatment plan we achieve long-lasting, permanent results if possible.
Recommended Reading: How To Get Rid Of Lower Back Pain Naturally
Treatment For Lower Back That Radiates To The Pelvis
Physical therapists generally perform extensive physical and diagnostic exams to make sure that the most beneficial treatment or therapy is recommended. The proper approach can help relieve acute pain in a short period of time. Of course, making an effort to adhere to the therapeutic plan will better help you overcome your pain and discomfort.
Individuals suffering from chronic lower back pain accompanied by discomfort in the front pelvic area may see dramatic improvement from physical therapy. This form of therapy is one of the most successful forms of pain management.
As a non-surgical approach, Physical Therapy is initially recommended for about 4-6 weeks to determine whether progress is being made or if a more invasive form of treatment, such as surgery, is needed. For some people, a longer physical therapy regimen results in long-term benefits.
The main goal of this type of therapy is to reduce inflammation, increase mobility, improve range of motion, restore muscle and vertebral function, and reduce or relieve back pain, which should target the pelvic pain at the same time. It is also important to target inflammation and irritation that may be affecting nerve roots in the lower back or pelvic region.
Physical therapists may even suggest the use of certain devices such as support belts, which offer extra support for the pelvis and lower back. A support belt helps reduce pain by stabilizing the sacroiliac joint as it easily wraps around the pelvis and hips.
Menstruation Or Uterine Dysfunction

Dysmenorrhea, a uterine dysfunction which is the origin of frequent and severe cramping for women during menstruation, also predisposes women to back pain. The condition is classified as either primary or secondary, and with both types, low back pain is a common symptom.
-
Primary dysmenorrhea begins when a woman starts her period and perpetuates throughout her life. Its harsh and atypical uterine contractions can result in recurrent and severe menstrual cramping.
-
Secondary dysmenorrhea usually begins later in life, and its caused by another condition such as endometriosis or pelvic inflammatory disease.
You May Like: How To Stop Lower Back Pain When Walking
How Is Sacroiliac Joint Pain Treated
Infographic:
If the pain is severe, assistive devices, such as walkers may be used. Sacroiliac belts may be worn temporarily for short periods in case of pelvic instability. Minimally invasive treatments, such as radiofrequency ablation may be considered in severe SI joint dysfunction. Rarely, SI fusion surgery may be recommended.3
If you suspect your SI joint to be a cause of your lower back pain, consult your doctor for a medical examination. A doctor can conduct specific clinical tests, rule out serious underlying conditions, such as tumors or infections, and formulate an effective treatment plan for your SI joint pain.