Symptoms Of Chronic Sciatica
The pain felt will mostly originate from the lower back and buttocks. It then radiates along the back of the thigh, moves past the knee, the calf at times, and the leg or foot. The pain is worse in the leg as opposed to the back.
Chronic sciatica pain may present itself as
- A mild to severe pain that some describe as shooting pain
- A severe burning sensation
- Numbness of the leg and foot
- A tingling sensation that feels like pins and needles in the leg and foot
Numbness and tingling should not be major causes for alarm unless they occur with foot drop or weakness of the leg muscles.
When one sits, more pain is felt because of the weight put on the intervertebral discs. Activities such as twisting and bending also worsen the pain but lying down will offer relief. One feels better when they run or walk, unlike when they sit or stand for long periods.
Good News Aboutvertebrogenic Back Pain
The good news for patients with vertebral endplate nerve dysfunction is that the condition can be treated with the new Intracept basivertebral nerve ablation procedure. Basivertebral nerve ablation is a minimally invasive treatment during which a spine doctor uses radiofrequency energy to destroy the nerve in the vertebral endplate that is transmitting pain signals to the brain.
The Intracept procedure is quick. I generally have patients heading home within three hours of arrival, and that includes recovery time. And it requires very little downtime afterwards. I recommend patients take it easy the rest of the day of the procedure, but then most patients can return to work and their regular routines the following day. The best part is, its long-lasting. Because the basivertebral nerve does not regenerate like other nerves in the body, patients dont need to worry about it growing back. And that means theres no need for repeat procedures. In fact, most patients pain continues to improve over time with the majority reporting 75% to 100% pain reduction five years after the procedure.
Top 11 Causes Of Chronic Low Back Pain
February 5, 2018 by Neurosurgical Associates of Central Jersey
Low back pain can really be a pain in thewell, back.
This condition is one of the most common health issues around. In fact, 31 million Americans experience low back pain at any given time, and it is the single leading cause of disability worldwide. In many cases, low back pain can resolve itself over a period of time. However, should the pain last longer than three months, it is then considered a chronic condition.
When chronic low back pain strikes, it can be due to any number of reasons. Lets take a look at some of the top causes of chronic low back pain:
Herniated discs.
Disc herniation occurs when the soft center of a spinal disc leaks through a crack in the tough exterior and places pressure on the surrounding nerve or nerve roots, resulting in pain. Herniated discs can happen in the cervical or lumbar sections of the spine.
Facet joint dysfunction.
Facet joints are joints that are located behind the majority of the spinal discs. They help give the spine its flexibility and stabilize it. When these joints become inflamed, they can cause pain similar to that of a herniated disc.
Spinal stenosis.
Spinal stenosis is a narrowing of the spinal canal where the spinal cord and nerves live. The narrowing can put pressure on the nerves, causing pain. Like disc herniation, this typically only occurs in the cervical or lumbar spine.
Spinal irregularities.
Also Check: Is Motrin Good For Back Pain
Less Common Causes Of Low Back Pain
While considerably less common, low back pain may also be caused by:
Infection. Also called osteomyelitis, a spinal infection is rare but can cause severe pain and is life threatening if untreated. It can be caused by surgical procedures, injections, or spread through the blood stream. Patients with a compromised immune system are more susceptible to developing an infection in the spine.
Tumor. Most spinal tumors start in another part of the body and metastasize to the spine. The most common tumors that spread to the spine start from cancer in the breast, prostate, kidney, thyroid, or lung. Any new symptoms of back pain in a patient with a known diagnosis of cancer should be evaluated for possible spinal metastasis.
Autoimmune disease. Back pain is a possible symptom associated with autoimmune conditions, such as ankylosing spondylitis, rheumatoid arthritis, lupus, crohns disease, fibromyalgia, and others.
This list includes the more common causes of back pain, but there are many more. Finding the optimal treatment for low back pain usually depends on obtaining a correct clinical diagnosis that identifies the underlying cause of the patients symptoms.
What Are Some Common Lower Back Pain Causes
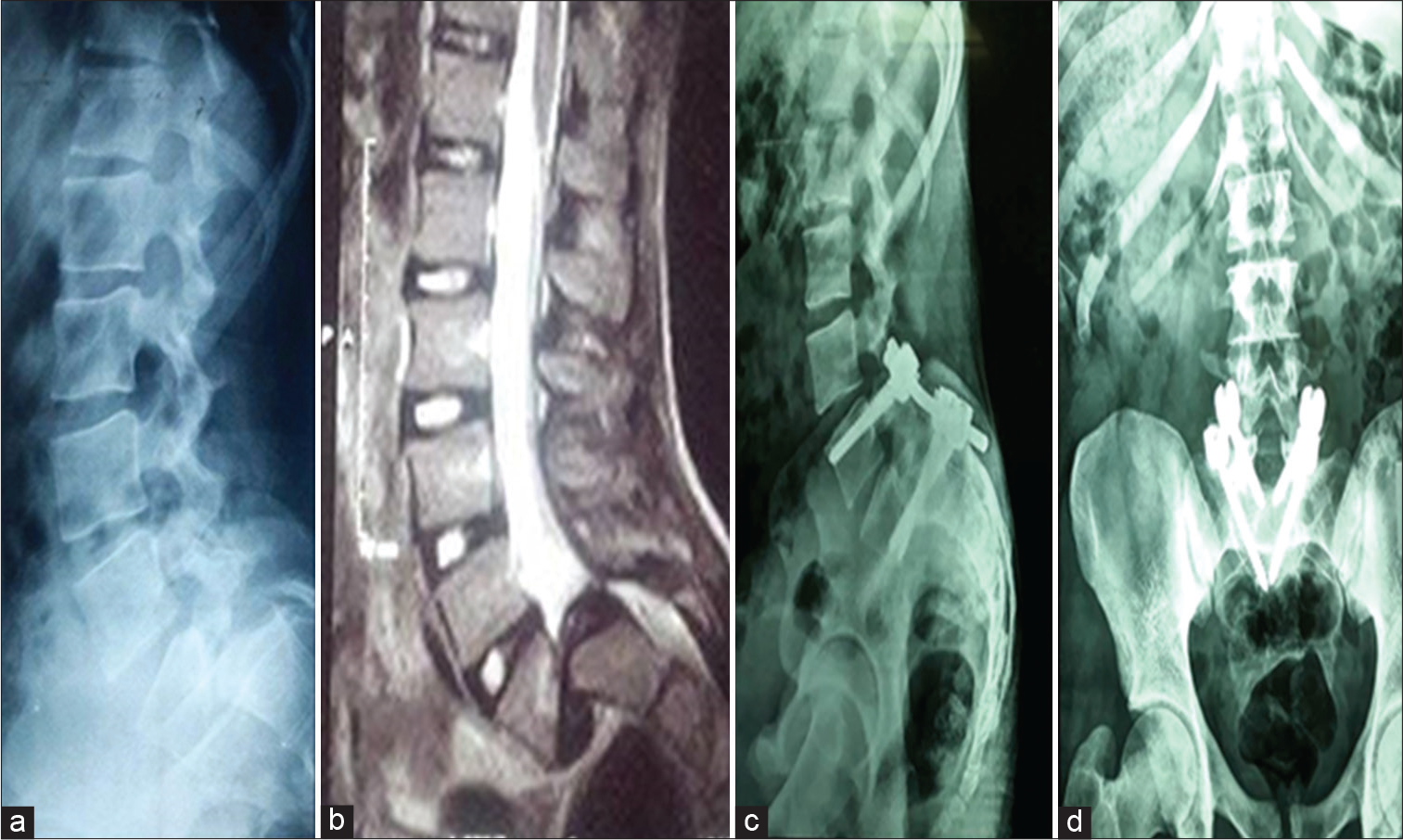
The causes of lower back pain are sometimes viewed as being mechanical, organic or idiopathic. Sometimes spinal conditions are congenital or acquired meaning the disorder develops later in life.
- Mechanical lower back pain is often triggered by spinal movement and involves spinal structures, such as the facet joints, intervertebral discs, vertebral bodies , ligaments, muscles or soft tissues.
- Organic lower back pain is attributed to disease, such as spinal cancer.
- Idiopathic refers to an unknown cause.
These are some of the things your doctor might look for or rule out when you schedule a visit for back pain.
The common symptoms of lower back pain.
Sprains and strains. Ligament sprains and muscle or tendon strains are the most common causes of lower back pain. Theyre often related to overuse.
Degenerative disc disease. While the name sounds worrisome, it just means you have a damaged disc causing pain. Over time, discs become thinner and flatter due to wear and tear. That leaves them less able to cushion the vertebrae and more likely to tear .
Herniated disc. The protective covering on intervertebral discs can tear over time. When this happens, the soft inner disc tissue may push through the outer layer. A disc that bulges or slips out of place is known as a herniated disc, bulging disc, or slipped disc. The herniation may press on nerve roots, leading to symptoms such as pain, tingling, numbness or weakness in the area that the nerve serves
You May Like: Is Advil Good For Back Pain
Neurophysiology Of Spinal Pain
Nociception is the neurochemical process whereby specific nociceptors convey pain signals through peripheral neural pathways to the central nervous system . Acute tissue damage to the spinal motion segment and associated soft tissues activates these pathways. When the peripheral source of pain persists, intrinsic mechanisms that reinforce nociception influence the pain. The nervous system can enhance a pain stimulus generated by tissue damage to levels far greater than any threat it signifies to the human organism this is a common clinical scenario in cases of chronic spinal pain.
Noxious mechanical, thermal, and chemical stimuli activate peripheral nociceptors that transmit the pain message through lightly myelinated A-delta fibers and unmyelinated C-fibers. Nociceptors are present in the outer annular fibrosis, facet capsule, posterior longitudinal ligament, associated muscles, and other structures of the spinal motion segment. Peripheral transmission of pain stimuli leads to the release of excitatory amino acids, such as glutamine and asparagine, which then act on N -methyl-D-aspartic acid receptors, causing the release of the neuropeptide SP. Neuropeptides such as SP, CGRP, and VIP are transported to the endings of nociceptive afferents, which inflammation and other algogenic mechanisms sensitize. Thereafter, the affected nociceptors respond to mild or normal sensory stimuli, such as a light touch or temperature change .
What Causes Lumbar Radiculopathy
You may get a pinched nerve in your lumbar spine if you have disc damage. Discs are natural, spongy cushions between your vertebrae that allow your spine to move. Your discs may move out of place and pinch the nerve in your spine. Your risk for a pinched nerve and lumbar radiculopathy increases if:
- You smoke.
- You have diabetes, a spinal infection, or a growth in your spine.
- You are overweight.
Read Also: Does Aleve Work For Back Pain
What Are Some Complementary Alternative And Emerging Treatments For Lower Back Pain
In some cases, doctors suggest therapies that are not considered standard of care. They probably wont be covered by insurance, but they may be worth considering. Examples include:
Platelet-rich plasma . PRP treatments use a small sample of your own blood that has concentrated amounts of blood building blocks known as platelets. Your doctor then injects the PRP directly into a damaged disc. The theory is that PRP injections use your own healing system to accelerate improvement of injured tendons, ligaments, muscles, and joints. PRP treatment has a longer track record in knee osteoarthritis, but a recent review article in the Journal of Spine Surgery suggests it may have a useful role for back pain, too. PRP needs a lot more research before it can be considered a proven technique.
Stem cells. In this emerging treatment, your doctor injects stem cells harvested from your hip into the intervertebral disc or discs causing your pain. Doing so may lessen pain and the degenerative effects of aging, though, like PRP, more research is needed before stem cells for lower back pain could eventually become the standard of care.
Acupuncture. Your doctor probably doesnt perform acupuncture , but may support you trying it as a complementary therapy. Acupuncture involves careful insertion of fine, sterile needles into specific points on your body. This may stimulate the release of your natural pain-killing chemicals.
Anatomy Of Your Spine
The low back, or lumbar spine, is composed of 5 bones that are stacked one upon another. Between the bones is a soft spongy disc. There is a joint on either side of your spine where one bone articulates with the ones above and below it. Your spinal cord and nerves are protected by these bones and discs. Many muscles and ligaments attach to the lumbar spine, giving it a combination of mobility and stability.
There are many nerves that originate in the low back. Some of these nerves stay in the low back, while some travel to other parts of the body, such as the buttocks or legs. Therefore, symptoms of low back problems can be felt in many places in the body.
This can make diagnosis and treatment of low back problems confusing and difficult. By monitoring where you feel the pain and understanding how your pain is changing, you can help your healthcare provider or physical therapist prescribe the best treatment for your low back pain.
Read Also: Aleve Lower Back Pain
Can Further Bouts Of Back Pain Be Prevented
Evidence suggests that the best way to prevent bouts of low back pain is simply to keep active and to exercise regularly. This means general fitness exercise such as walking, running, swimming, etc. There is no firm evidence to say that any particular back strengthening exercises are more useful to prevent back pain than simply keeping fit and active. It is also sensible to be back-aware. For example, do not lift objects when you are in an awkward twisting posture.
Mechanical Versus Nonmechanical Spinal Disorders
Mechanical syndromes
-
Diskal and facet motion segment degeneration
-
Muscular pain disorders
-
Diskogenic pain with or without radicular symptoms
-
Radiculopathy due to structural impingement
-
Axial or radicular pain due to a biochemical or inflammatory reaction to spinal injury
-
Motion segment or vertebral osseous fractures
-
Spondylosis with or without central or lateral canal stenosis
-
Macroinstability or microinstability of the spine with or without radiographic hypermobility or evidence of subluxation
Nonmechanical syndromes
-
Myelopathy or myelitis from intrinsic/extrinsic structural or vascular processes
-
Lumbosacral plexopathy
-
Acute, subacute, or chronic polyneuropathy
-
Mononeuropathy, including causalgia
-
Myopathy, including myositis and various metabolic conditions
-
Spinal segmental, lumbopelvic, or generalized dystonia
Systemic disorders
Osseous, diskal, or epidural infections
Inflammatory spondyloarthropathy
Metabolic bone diseases, including osteoporosis
Vascular disorders
Referred pain
Gastrointestinal disorders
Cardiorespiratory disorders
Disorders of the ribs or sternum
Genitourinary disorders
Thoracic or abdominal aortic aneurysms
Hip disorders
Read Also: Advil Vs Ibuprofen For Back Pain
Looking For The Pain Generator
Imaging findings are weakly related to symptoms. In one cross-sectional study of asymptomatic persons aged 60 years or older, 36% had a herniated disc, 21% had spinal stenosis, and more than 90% had a degenerated or bulging disc.
Although it is not possible to gauge accurately, it is easy to believe that these conditions could have a yearly cost, directly and indirectly, of more than $50 billion and conceivably up to $100 billion. A recent study estimated that lumbar radiography was performed 66 million times in the United States in 2004, with a cost of $54 for each exam. Although estimates vary substantially depending on geographic location, insurance status, and other factors, costs of MRI seem to be 10 to 15 times higher,.
The most recent guidelines for clinicians suggest that when faced with LBP patients, the clinician should go through a careful diagnosis of the mechanisms that sustain acute and/or chronic pain. Treatment has to be addressed specifically to these mechanisms. In this manner, we could avoid the common mistake of making the diagnosis of simply low back pain, resulting in improper treatment of a definition and not a complex disease. As chronic LBP could have simultaneous multiple pain generators, a multi-disciplinary diagnosis and multimodal treatment is necessary.
Referred Pain To And From The Lumbar Spine
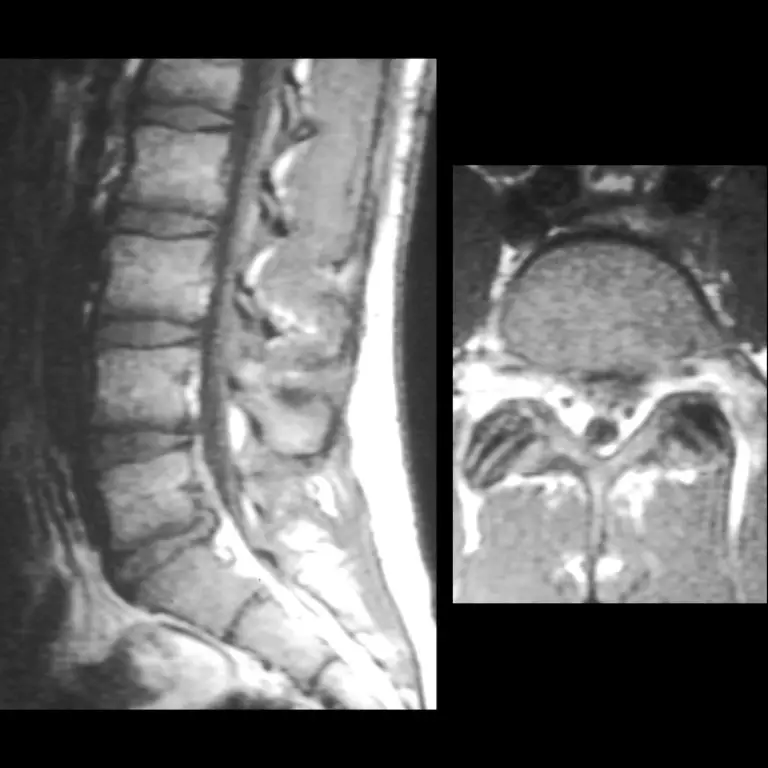
Pain in the area of the lumbar spine may be due to important problems that are actually unrelated to the back. Referred pain occurs when a problem in one place in the body causes pain in another place. The pain travels down a nerve.. Sources of referred pain to the low back may include abdominal aneurysm , tubal pregnancy, kidney stones, pancreatitis, and colon cancer. Clues to these maladies include pain that waxes and wanes over a short period, with frequent peaks of intense pain, weight loss, abnormalities found during abdominal exam, and trace amounts of blood in the urine. On the other hand, pain can be referred from the low back and be felt in another location, as is often the case with . For example, it is not rare for a patient with a slipped disc in the lower back to have pain in the back of the thigh, or in the calf or even the foot, and not have any low back pain. This situation requires a doctor to sort out the type of pain and to do the examination required to show that the pain is actually coming from the spine .
You May Like: Mayo Clinic Lower Back Pain Exercises
Evolutionary Mechanisms In Chronic Lbp
Chronic LBP is not the same as acute LBP that persists for a greater duration. Usually 6-7 weeks is sufficient for healing to occur in most soft-tissue or joint injuries however, 10% of LBP injuries do not resolve in this period. The evolution of cLBP is complex, with physiological, psychological, and psychosocial influences. These influences can be divided into 3 major categories, with subcategories, as follows:
-
Neurophysiological mechanisms
Social
The Big Three Signs That You Should Investigate For An Ominous Cause Of Persistent Low Back Pain
You shouldnt worry about low back pain until three conditions have been met:
The presence of the big three does not confirm that something horrible is going on. It only means that you need to check carefully.
Andy Whitfield as Spartacus
At his physical peak, not long before getting sick. The first sign of his cancer was steadily worsening back pain. He may have already been in pain at this time.
The story of actor Andy Whitfield is a disturbing and educational example of a case that met these conditions for sure the first two, and probably the third as well if we knew the details. Whitfield was the star of the hit TV show Spartacus . The first sign of the cancer that killed him in 2011 was steadily worsening back pain. Its always hard to diagnose a cancer that starts this way, but Whitfield was in the middle of intense physical training to look the part of historys most famous gladiator. Back pain didnt seem unusual at first, and some other symptoms may have been obscured. Weight loss could have even seemed like a training victory at first! It was many long months before he was diagnosed not until the back pain was severe and constant. A scan finally revealed a large tumour pressing against his spine.
Is back pain a symptom of COVID-19?
You May Like: Does Aleve Help Back Pain
Lower Back Pain Causes
Nonspecific low back pain means that the pain is not due to any specific or underlying disease that can be found. It is thought that in some cases the cause may be an over-stretch of a ligament or muscle. In other cases the cause may be a minor problem with a disc between two spinal bones , or a minor problem with a small facet joint between two vertebrae. There may be other minor problems in the structures and tissues of the lower back that result in pain. However, these causes of the pain are impossible to prove by tests. Therefore, it is usually impossible for a doctor to say exactly where the pain is coming from, or exactly what is causing the pain.
To some people, not knowing the exact cause of the pain is unsettling. However, looked at another way, many people find it reassuring to know that the diagnosis is nonspecific back pain which means there is no serious problem or disease of the back or spine.